Implanted Heart Rhythm Devices
APR 08, 2024A healthy lifestyle is very important to protect the electrical system of the heart. Once it gets damaged, the heart may have little ability to recover.
Read More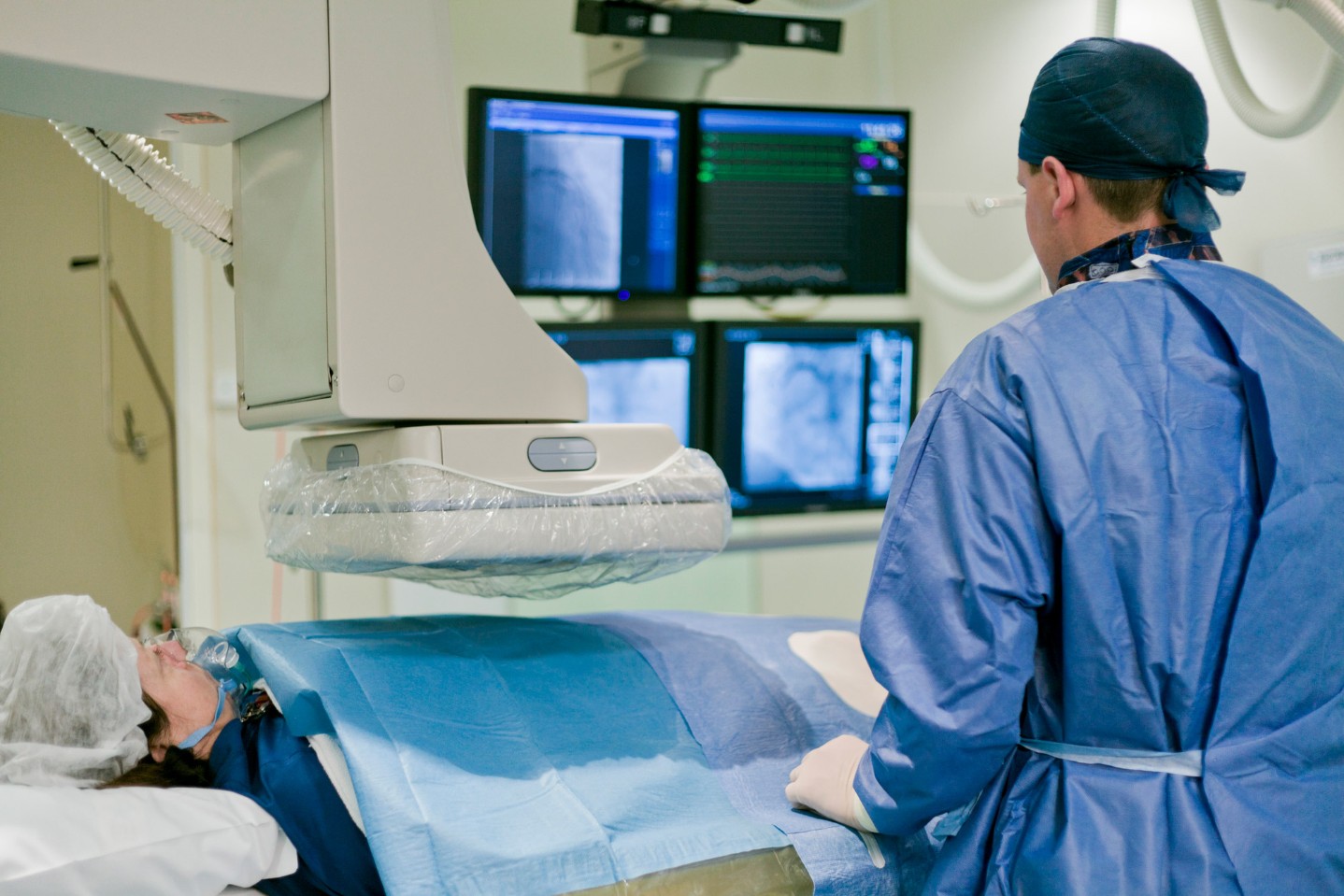
When I recommend that a patient needs coronary angiography (synonyms: heart catheterization, coronary angiogram, cardiac catheterization, or simply “cath”) I take a moment to bring up the risks of the procedure—complications that include the rare likelihood of stroke or heart attack (less than one in a thousand), a reaction to the dye, and bleeding at the arterial access site (most often the femoral artery in the groin).
Patients are appropriately concerned about the risks of this invasive procedure (especially when they see my diploma on the wall from the Medical School of the Caribbean and my certificate of membership to the Holiday Inn Express travelers club). We who perform many cardiac catheterizations a year are also realistically cautious, since simple mathematics dictate that we will face even rare adverse consequences if we do enough of these (a one-in-a-thousand occurrence sounds like remote odds until you consider thousands are done in Omaha each year).
Before patients get too worked up about the uncommon complications of the routine diagnostic coronary angiogram (I’ve heard it said that no procedure is routine if it’s being done to you) they should consider how far we’ve come.
Last year marked the 50th anniversary of the coronary angiogram. A history of the development of this test is nicely outlined in an article from Journal of the American College of Cardiology entitled “A Half Century of Selective Coronary Arteriography.”
Before we turn to a chapter from history, here’s a brief tutorial on how we do it these days. The cardiologist starts by feeling for the pulse in the groin that indicates the presence of the femoral artery, then numbs the skin and places a sheath (I.V.-like tube) into the vessel. The doctor passes a catheter through the sheath up through the aorta and inserts the tip into the opening of the coronary arteries. Different shapes of catheters allow us to easily locate the arteries despite considerable variability in the anatomy of individuals (I use the adverb easily when describing this, but I confess that the word easily rarely came to mind when I was in fellowship training trying to located the origin of the right coronary artery).
We inject a few milliliters of iodine-based dye into the artery and film the whole thing with an x-ray camera. It’s at that point where a lot of our patients (those not drifting off to sleep) can see their arteries appear on the TV screen, although to the untrained eye the arteries look somewhat like the silhouette of a gnarled oak tree.
The coronaries are not 2-dimensional structures, and until James Cameron comes out with some cool 3-D cath lab glasses we are stuck trying to visualize this complex web of arteries on a flat-screen monitor. To help with this we shoot many different views of the same arterial tree—we image from the hips up toward the opposite shoulders (and vice-versa) and can shoot straight-on or sideways—using an x-ray camera that has the ability to swivel around to nearly any position we want.
Almost immediately we can tell if there is a blockage and what needs to be done. From there we proceed to angioplasty and stent placement or bypass surgery if needed. The whole process can be done in as little as 10-15 minutes.
While the history of coronary angiography stretches back 50 years, the use of catheters in human blood vessels came several years earlier. Werner Forssman, an imaginative but somewhat disobedient German medical student, hatched the idea that a catheter could be passed from a peripheral vein into the heart for the purpose of diagnosing and treating heart problems. The department chief resolutely dismissed the idea—getting anywhere near a beating heart was long believed to be an invitation for disaster. Finding no other suitable volunteers, Forssman simply anesthetized his own arm, inserted a catheter into the vein and snaked it toward his chest. Legend has it that a nurse who tried to stop him was thwarted by Forssman who strapped her to an operating table. These days that kind of behavior would get you tossed from the hospital staff—back then they rewarded him the Nobel Prize in medicine.
Now let’s skip ahead in time to the accident that launched the entire specialty of invasive cardiology. In 1958 a young cardiologist named Mason Sones prepared to perform a routine imaging procedure on a 26-year-old patient with rheumatic valvular heart disease. In those days it was pretty common to pass a catheter into the root of the aorta and inject a big blast of dye—let it spread through all the vessels of the chest while filming with an immense x-ray camera. With this technique a reasonable view of the coronary arteries was obtained, but detailed imaging remained outside the realm of possibility. On that day the catheter tip inadvertently slipped into the opening of the right coronary artery just as the full volume of dye was injected.
Up until that point it was widely believed that injection directly into a coronary artery would lead to certain cardiac arrest and death. Dr. Sones, upon realizing what had just happened, “leaped up from the pit and grabbed a scalpel to open the chest and perform open cardiac massage.” The “pit” where Dr. Sones stood was a trench under the cath table that was needed to house the massive and thoroughly immobile x-ray equipment (In contrast to our current technique where the camera is rotated around the patient, the original design required that the patient be spun and pivoted around the fixed x-ray camera—the patient was strapped to the table and spun around like a NASA recruit. I am unable to locate any first-hand patient reports of this experience, although I wouldn’t be surprised if they were admonished to keep their hands and feet inside the ride at all times.).
Much to the surprise of Dr. Sones and his staff the patient suffered no more than a brief slowing of the heart rate and a rapid recovery. That moment spelled the demise of the myth of the deadly dye injection. From that day on we have comfortably injected gallons of dye into the arteries of millions of patients with considerably less excitement.
Nowadays during routine angiograms we rarely leap onto the chest of our patients with scalpel in hand (I did this only twice last week) or tie nurses to OR tables (any comment I add here will likely just get me in trouble). The procedure these days takes only about 15 minutes and uses only a small amount of dye, and, thanks to the magic of conscious sedation, we’re often finished before the patient even knows we started.
From my perspective as a doctor, we’ve come a long way and ended up with a procedure that is thankfully pretty dull and uneventful. For the patient, decades of refinement and experience among the cardiology community have produced an imaging study that is remarkably safe and effective.
Over the next 50 years we’ll probably find ways to open blocked vessels without ever needing to puncture the skin or enter the heart—no more needles, x-rays, or contrast dye. No more leaping onto the table with a scalpel or tying nurses to tables. It seems like a great move in the right direction even if it is a little less exciting.

A healthy lifestyle is very important to protect the electrical system of the heart. Once it gets damaged, the heart may have little ability to recover.
Read More
Heart disease is the number one cause of death for women and men, claiming more lives than all forms of cancer combined.
Read More
With heart disease remaining the number one killer of women and men in the United States, it’s important to take action to protect your heart – even if you feel fine.
Read MoreWhen you need local health information from a trusted source, turn to the CHI Health Better You eNewsletter.