Conquer the Crushing: Understanding and Managing Migraines and Headaches
JUN 19, 2025Understanding the type of headache you're experiencing is crucial for effective treatment.
Read More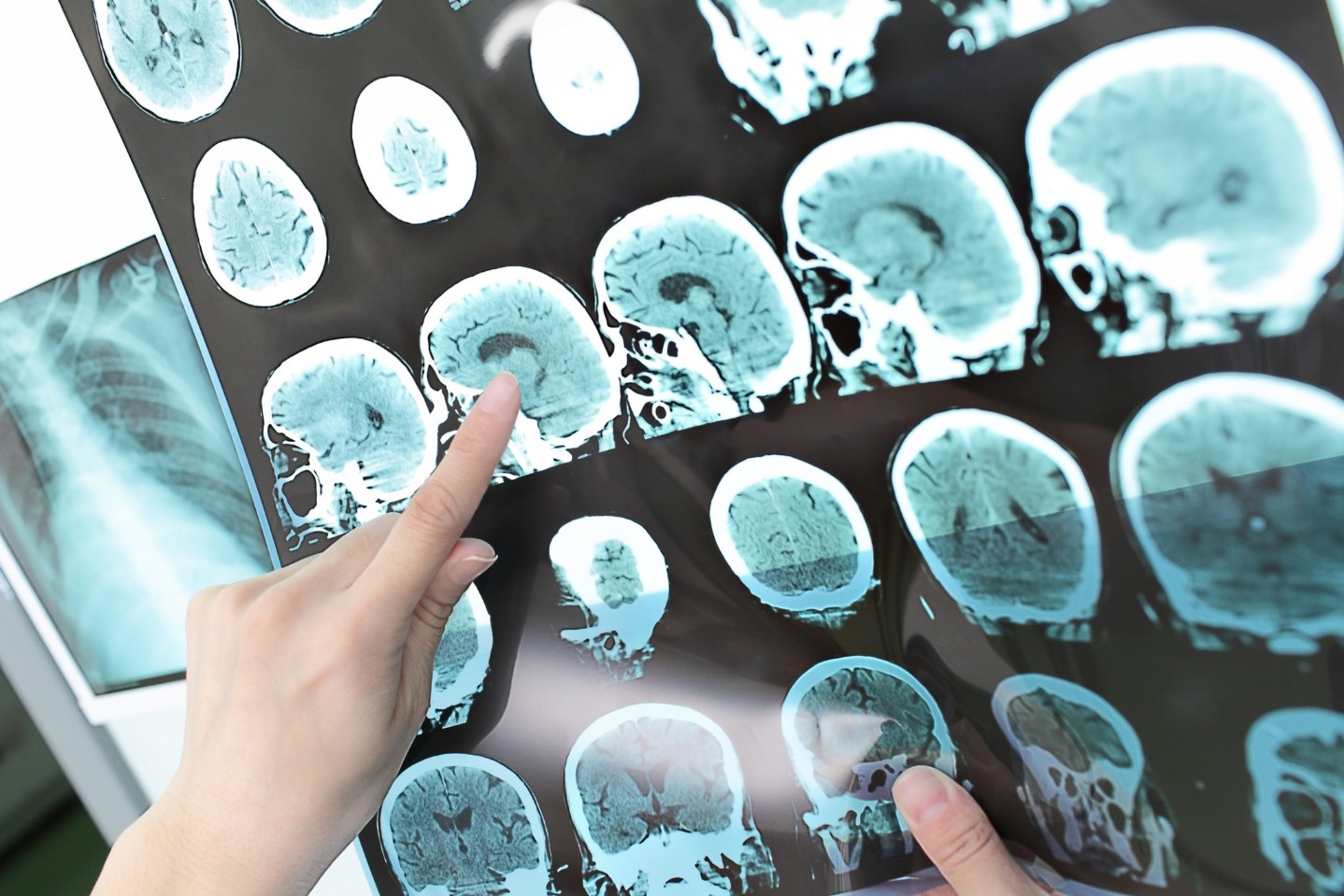
Nearly 1 million adults in the U.S. are living with multiple sclerosis (MS), according to the recent MS Prevalence study sponsored by National MS Society. This central nervous system disease affects the brain, spinal cord and optic nerves in the eyes.
Unpredictability is the hallmark of multiple sclerosis (MS) because symptoms range from minor to debilitating – and progression can be slow or rapid.
Multiple sclerosis is an autoimmune disease that causes your immune system to attack the central nervous system and damage the coating around nerves (myelin) with subsequent neuronal damage as well. This damage disrupts the sending and receiving of messages in the brain and between the brain and the body – resulting in symptoms which can affect vision, balance, muscle control and other bodily functions.
Some of the less common symptoms include speech and swallowing problems, tremors and seizures, breathing problems and hearing loss.
Most people are diagnosed between the ages of 20 and 50. There is no single test for MS, so the diagnostic process generally involves a thorough medical history, a neurologic exam and tests including an MRI, spinal fluid analysis and blood tests which rule out other conditions. Diagnosis requires evidence of damage in two separate areas of the central nervous system. Plus, evidence that damage occurred at two different times.
What causes MS remains unknown. Researchers believe a combination of factors may be involved and are currently studying genetic, infectious, immune system and environmental factors. They have determined that women are more than two to three times as likely as men to have MS. A family history of MS puts you at a little bit higher risk of developing the disease.
Treating multiple sclerosis is an individual process because each case is different. There is no cure, but much can be done to manage symptoms, aid recovery from attacks and slow disease progression. Treatment options include oral and injectable medications and infusions treatments. Physical therapy can also help with MS symptoms.
For some, symptoms are mild and require no treatment. Close monitoring is necessary as disease progression can occur without obvious physical symptoms.
Historically, multiple sclerosis has been difficult to treat because there were no available treatment options before 1990's. The good news for those with MS is there are multiple new medications that have been approved since then, which have shown promise in slowing the progression of the disease. In fact, most of them that were approved were for the most common, relapsing-remitting form of MS.
In 2017 and 2019, two new medications were introduced for the treatment of MS. These medications were approved in the area in which previously we didn’t have medication options, and were also approved for relapsing-remitting forms of MS
While none of these medications are considered a cure, with early initiation, therapy can really change the disease course significantly. The bottom line is people with MS now have more hope and much better chances for good outcomes.
If you have questions or feel you need to be tested for MS, reach out to your provider.

Understanding the type of headache you're experiencing is crucial for effective treatment.
Read More
Proper diet is essential in maintaining bladder and bowel health as they affect your gut microbiome.
Read More
Injuries spike during the summer months but there are actions you can take to prevent injuries during the 100 deadliest days of summer.
Read MoreWhen you need local health information from a trusted source, turn to the CHI Health Better You eNewsletter.