Be a Lifesaver: It's National CPR and AED Awareness Week!
JUN 02, 2026Cardiac arrest is when the heart suddenly stops beating effectively, preventing blood from flowing to the brain and other vital organs.
Read More
Restless Leg Syndrome (RLS) also known as Willis Ekbom Syndrome, is characterized by an uncomfortable need to move your legs, primarily at night while trying to sleep.
It is present in 2-3% of the general population, more common in women, and the Caucasian population.
My patients often tell me that it is hard to describe the way their legs feel. I’ve heard the leg sensation described as anything from “creepy crawlies on my legs” to “feeling I have to go run.” Occasionally, the patient’s spouse or bed partner complains about being kicked frequently at night.
A quick way to see if you possibly have RLS, is using the acronym URGE.
The first thing I ask my patients when they come into my office with these symptoms, is “How much caffeine do you take in?” Some of the first things we check for that could be causing RLS include:
I usually ask my patient to cut out ALL caffeine/tobacco use and the medications described above (if safely possible) prior to doing further testing. If they still have persistent symptoms, I consider other causes.
RLS can be a caused by other underlying medical disorders including Iron Deficiency, Renal Failure, Parkinson’s disease, Multiple Sclerosis, Pregnancy and Spinal Cord Disorders. Thus, it is important to rule some of these out.
Frequently, providers check a ferritin levels, which is an indicator of Iron stores. A quick fix to cure RLS symptoms is iron supplementation, especially if ferritin levels are low.
If my patient still has symptoms, and blood work is normal, I consider medication used specifically to treat RLS. If you have RLS symptoms, try implementing some of the above changes mentioned, it could save you a trip to the doctor's office.
To learn more about other sleep disorders that might be keeping you awake at night, please visit our Sleep Disorder Services.
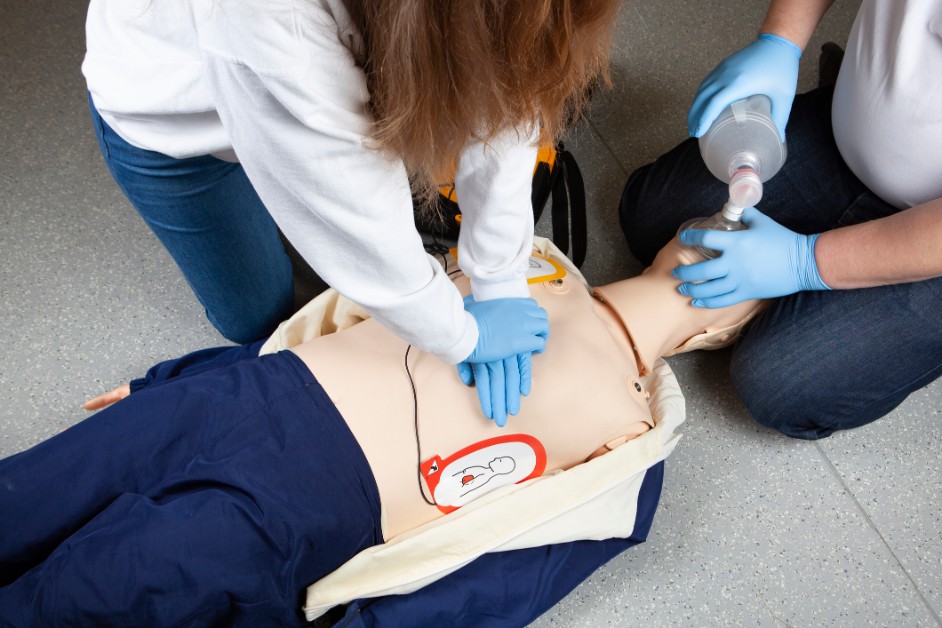
Cardiac arrest is when the heart suddenly stops beating effectively, preventing blood from flowing to the brain and other vital organs.
Read More
Low-dose radiation therapy is an effective treatment designed specifically for chronic arthritis pain, particularly for hip, knee and hand osteoarthritis.
Read More
High blood pressure (hypertension or HTN) is the number one preventable risk factor for heart disease and death worldwide.
Read MoreWhen you need local health information from a trusted source, turn to the CHI Health Better You eNewsletter.