Dr. Frederick Frankenstein: [to Igor] Now that brain that you gave me. Was it Hans Delbruck's?
Igor: [pause, then] No.
Dr. Frederick Frankenstein: Ah! Very good. Would you mind telling me whose brain I DID put in?
Igor: Then you won't be angry?
Dr. Frederick Frankenstein: I will NOT be angry.
Igor: Abby Someone.
Dr. Frederick Frankenstein: [pause, then] Abby Someone. Abby who?
Igor: Abby Normal.
Dr. Frederick Frankenstein: [pause, then] Abby Normal?
Igor: I'm almost sure that was the name.
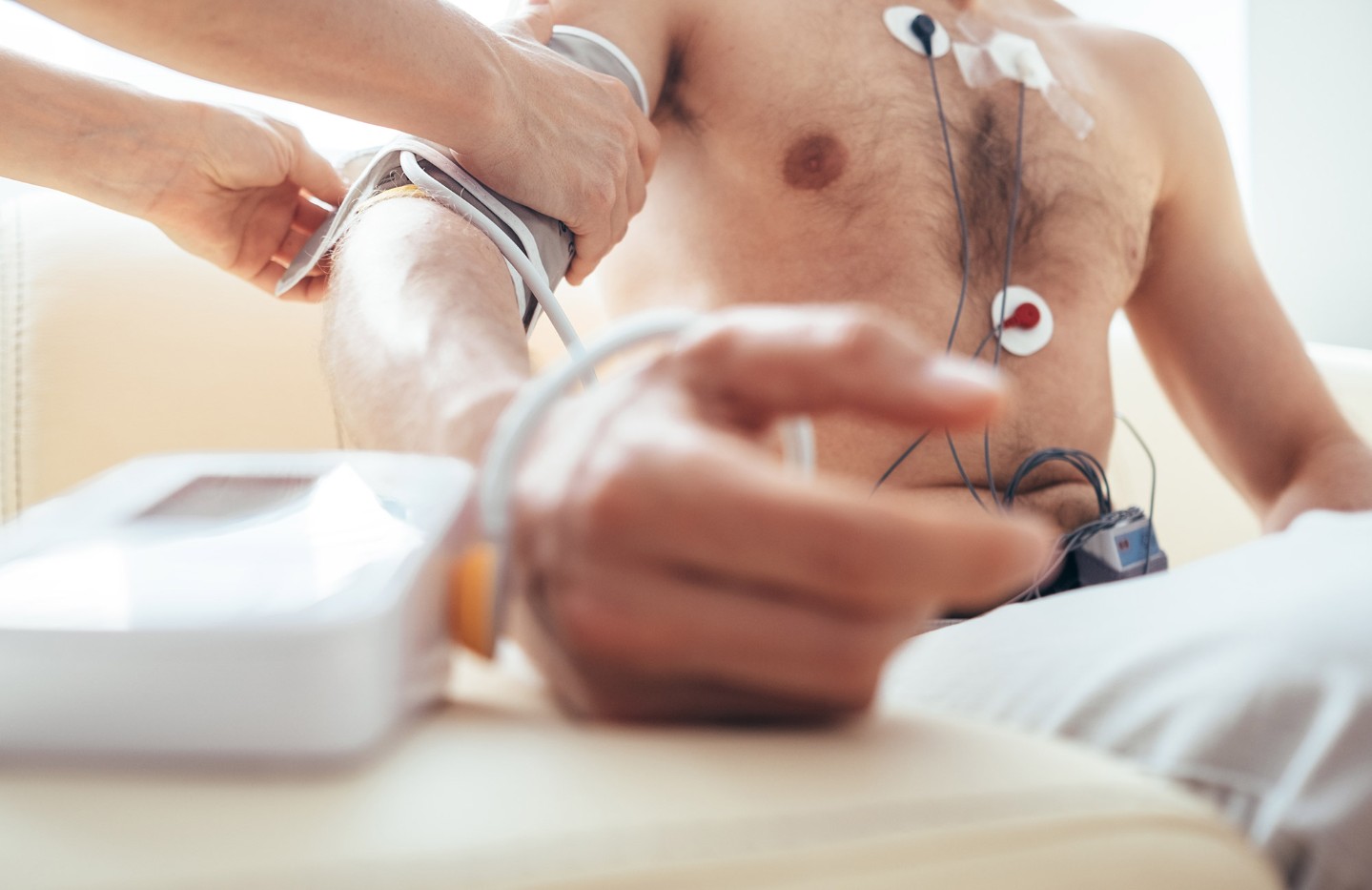
I saw a very anxious guy the other week who was sent to me for evaluation of an abnormal electrocardiogram (EKG). His health was good and he got an EKG as part of a routine physical exam. The computer in the EKG machine interpreted the abnormality as an “incomplete right bundle branch block,” a pretty frightening mouthful of scary words for a nonmedical person, and my nonmedical patient was plenty upset.
After I provided a normal exam and echocardiogram I could reassure him that he just might survive his brush with death. My problem came when I suggested that his EKG abnormality represented something that I (and most cardiologists) see as essentially normal. “Normal?” He responded, “How can a blockage be normal?”
So, the first thing I did was to launch into a brief lecture on the cardiac electrical conduction system (for those of you who are interested, see below*). The second thing I did was start thinking about what actually constitutes “normal” in the medical world.
In medical school I learned how laboratory “normals” are set. These are the numbers that represent the range where presumably normal patients fall. For example, if you get your hemoglobin measured in one of our Alegent labs you’ll be provided with your result accompanied by a range of normals (13.5 - 17.5 gm/dl). If you have a hemoglobin level of 13.5, you’re normal; if it’s 13.4, you’re not (and are thus mildly anemic).
To determine the reference range for any laboratory value you first need a few thousand presumably healthy volunteers. You draw blood from all of them and measure whatever you’re looking for—as an example let’s use a made-up blood component we want to assess, say “midi-chlorians”. You find that your healthy subjects have a wide variety of midi-chlorian levels, some high, some low, most of them right in the middle. Now comes the magic of statistics. You figure out what level of midi-chlorians the bottom and top 2.5% of subjects have. Then you simply take the middle 95% of values and label them normal, and those at the highest and lowest levels become the abnormals. If the reference range for midi-chlorians is 4.5 to 178.9 mJjb (millijarjars)—implying that 95% of the normal population fall into this span—then someone with a level of 180 mJjb would be defined as abnormal, even if the specimen came from one of your normal volunteers.
And, as everyone knows, one’s midi-chlorian level is fixed from birth. What about bodily components that change over time? The b-type natiuretic peptide (BNP), for example, is a protein marker of congestive heart failure that rises steadily with age and varies according to gender and level of obesity. A “normal” BNP for you at age twenty (when you can still fit into those skinny jeans) may not be the same when you are twice that age (and maybe twice that size), even if you consider yourself to still be normal.
Another issue relates to tests where there is debate about what should be considered normal. The best example in this category is LDL cholesterol (LDL-C). Pull in a thousand random healthy volunteers from the U.S. and you’ll find that the average LDL-C is around 130 mg/dL. Does that mean that 130 mg/dL should be the standard for what is normal? What if our supposedly “healthy” volunteers aren’t so healthy after all? Just because the average LDL-C in this country is 130 mg/dL doesn’t necessarily mean that this represents the level at which our bodies function most normally.
Lipid researchers have long postulated that the LDL-C levels in our society are anything but normal. We’ve long known that LDL-C rises with age in our society despite the fact that this is actually not a normal phenomenon. Consider this paragraph from a review entitled “Redefining Normal Low-Density Lipoprotein Cholesterol” in a recent edition of Journal of American College of Cardiology:
“At least two adult human populations, however, do not exhibit this progressive increase in LDL-C with age. One population consists of hunter-gatherer societies, diverse in geographic location and ethnic origin but arguably living the way humans did 10,000 years ago. LDL-C levels remain in the 35 to 70 mg/dL range. In modern societies, rural Chinese blood levels often fall within this range. In neonates and these two adult groups, atherosclerotic coronary disease is rare. The consistency of these diverse human data sources, taken together with the mammalian species data, supports the speculation that the putative normal range of LDL-C in adult humans may be approximately 35 to 70 mg/dL.”
Sure, 130 mg/dL of LDL-C is typical in our population, but what would it be if we didn’t spend 90% of our lives subsisting on fast food and exercising as much as catatonic tree sloths? In the case of LDL-C, normal is likely less than 70 mg/dL and anything much above that (in other words, nearly all of us) falls in the abnormal range.
Another good example of a test with a gray demarcation between normal and abnormal is the echocardiogram (ultrasound evaluation of the heart). Strictly speaking, a normal echocardiogram would be one where all structures look like they do in the anatomy textbooks and all valves open and close like doors of an expensive German sedan. With those criteria in mind we’d have to conclude that the finding of valve leakage constitutes an abnormal result. Those of us who routinely read echocardiograms, however, will tell you that nearly all people have some degree of valve leakage. Furthermore, there is a long laundry list of structural aberrancies that are both abnormal and of absolutely no relevance. The nurses in our office—who are routinely tasked with calling patients to notify them of test results—struggle with this issue all the time. The report says “mild tricuspid regurgitation, diastolic dysfunction, and estimated pulmonary pressure of 40 mmHg”—all abnormal findings, but almost expected in the geriatric population—and what are they to tell the patient? They can’t say that the echocardiogram is normal but they also shouldn’t alarm the patient with news of something that has absolutely no clinical relevance.
In a recent blog post I wrote about the idea of providing patients with their own copies of the medical record that accompanies their office visits. Some physicians have expressed concern about anxious patients focusing on test results that are abnormal but not relevant. Will a patient be concerned if they discover that their hemoglobin is 17.6 gm/dL (one-tenth of a point higher than the normal range) after their doctor glosses over this as if it’s meaningless?
Maybe we need three categories instead of just two: normal, abnormal but benign, and abnormal/concerning (or something like that). We could adopt the Homeland Security model and provide a color-coded threat assessment (“your hemoglobin is threat level green but your midi-chlorians are deep in the orange range”).
It’s clear that there are many things in the world of medicine where abnormal does not necessarily equate to problematic. The real difficultly lies in the fact that human beings have so many inherent variations and that normal human physiology can proceed despite small aberrancies from the norm. Most patients are sophisticated enough to understand this concept but for others we doctors may just have to devote a little more effort in education and communication. My patient with the EKG abnormality left the office perfectly satisfied and at ease after a discussion that took only a couple of minutes out of my day.
Finally, you may be wondering about my opening quote from the classic 1974 movie Young Frankenstein and what, if anything, it has to do with the subject of this post. Well, don’t think about it too much. I guess it’s just another proof that seemingly normal things (such as blog-writing cardiologists) can be abby normal and still remain somewhat functional.
* Brief Primer on Cardiac Conduction:
Electrically speaking, the top chambers of the heart (the atria) are connected to the bottom chambers (the ventricles) by specialized tissue that acts like two electrical wires. One wire, the left bundle branch, sends electrical stimulus to the left ventricle, while the right bundle branch stimulates the right ventricle. Since the two ventricles are attached to each other, only one of the two branches is required for an electrical impulse to stimulate both ventricles to contract. If a healthy person loses function of one of the two branches his/her heart will continue to function normally without missing a beat (pun intended). The likelihood of losing function of both branches is remote.
A right bundle branch block (RBBB) is present as a “normal” finding in about 1% of people under the age of 50 and in about 10% of people over the age of 80. An incomplete RBBB (as in the case above) implies slow function—but not complete loss—of the right branch and is relatively common in young, healthy individuals. It has no clinical significance.
The fact that the word “block” is used to discuss both electrical and arterial problems is unfortunate and sometimes confusing. The block in RBBB and LBBB refers only to absence of electrical conduction and does not relate to blockage of blood flow.